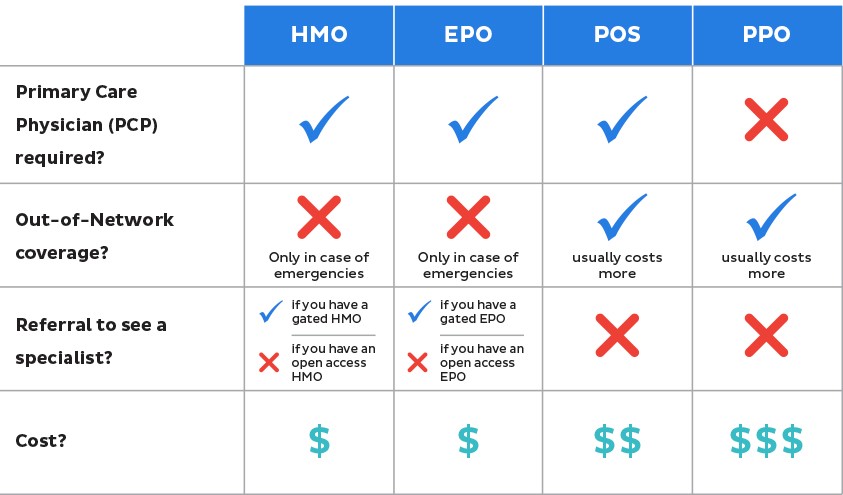
The plans additionally expect people to pick a primary doctor who decides the type of treatment patients need. This implies that somebody who gets clinical benefits out of the HMOs network should pay for it themselves. The plan may likewise expect people to live in a specific region. For example, HMOs only permit insured parties to see people in their own network, which implies that they are answerable for the full amount of a visit to any specialist or doctor outside this group. There are a few limitations for those covered under HMOs, which is the reason why these plans have a bad reputation. Recommended Reading: What Happens If My Health Insurance Lapses Why Do Hmos Have A Bad Reputation With this plan, you get complete medical, hospital, and Part D Prescription Drug coverage and you can see out-of-network doctors for all covered medical services, though you pay less for in-network doctors. Generations Advantage Select is designed for those looking for a health care plan with more flexibility. Platinum PPOs have a potential for increasing consumer costs because they treat outside resources with lower cost sharing, and they do not count outside network spending towards the deductible and expense limits. The division of cost sharing is ninety percent to ten percent for the customer. The deductibles are reachable ad the overall limits are within usual ranges. Platinum PPO plans offer high degrees of coverage for network resources. The Marketplace offers the below-described types of PPO plans Many consumers can decide that they prefer PPO plans for the greater range of choices rather than HMO for the slightly lower costs. The type of managed care is also an important similarity. The four types of Marketplace plans use actuarial value to group them. In addition, PPOs are generally more expensive because they give you more freedom of choice in terms of the medical providers you can use. Some require a primary care physician to act as your gatekeeper, only allowing you to get healthcare services with a referral from your PCP others dont. Some have minimal cost-sharing others have large deductibles and require significant coinsurance and copays. Some pay for out-of-network care some don’t. Managed-care plans like HMOs, exclusive provider organizations and point-of-service plans differ from PPOs and from each other in several ways. Related Articles : The Difference Between A Ppo And Other Types Of Health Insurance For example, if a doctor charges $100 for a consultation, then the copay would be $2. 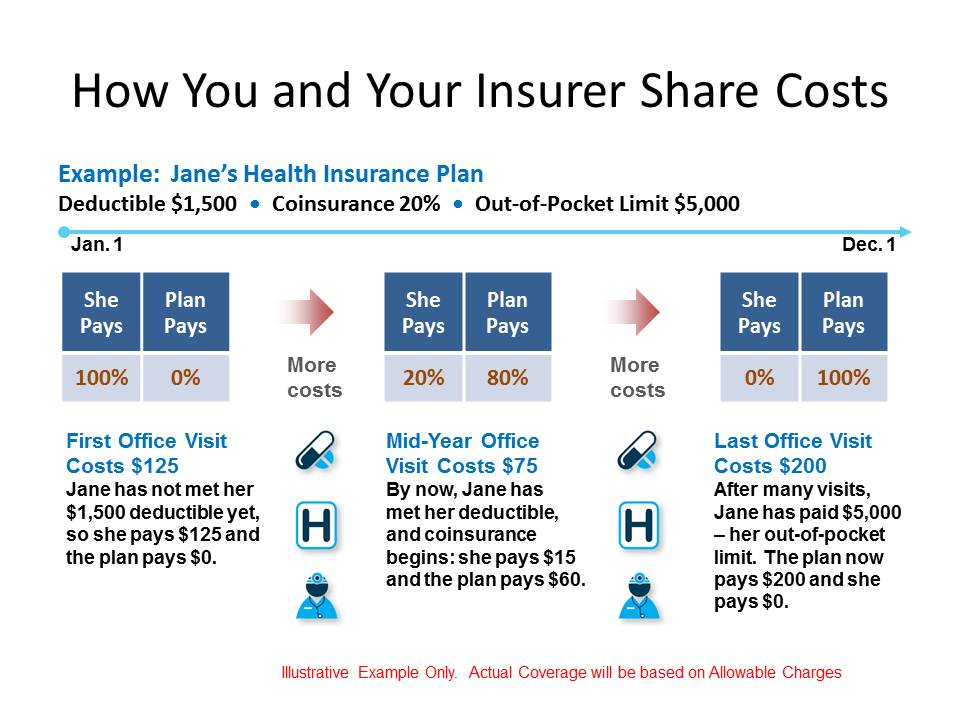
Copay is an amount of money that the insured person will pay before insurance coverage can be obtained. If a person pays part of the cost of their medical treatment, the payment is considered copay. Copay or co-pay is a reimbursement term used by health insurance providers to describe the amount of an uncovered medical expense that must be paid out-of-pocket prior to coverage beginning. If your doctor charges a copay, then you simply need to pay the copay fee each time you visit. 
“Copay” is a term that’s used to describe the amount of money that you have to pay each time you go to the doctor. For example, a customer might be charged $50 for the first visit and $25 for the second visit. The copay amount is typically charged per purchase in order to create a tiered arrangement. Copay is a pricing term that refers to the cost of an item in relation to the number of items purchased. It may also be used to cover the cost of other services or medications. 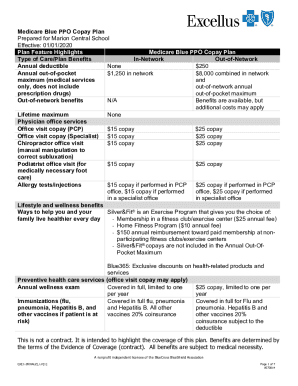
It is a payment requested from your insurance provider for a medical service or prescription drug that requires a co-payment.Ĭopay can vary depending on the plan and may be required before the service or medication is provided. The copay is the amount of money that a patient has to pay out-of-pocket for certain medical treatments or procedures, such as surgery and doctor visits.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
